Rectal Cancer Treatment
Rectal cancer is a serious but treatable disease when detected early and managed with the right medical approach. The rectum is the last part of the large intestine, located just before the anus. Cancer that develops in this area is called rectal cancer. Because this part of the body plays an important role in passing stools, rectal cancer can cause distressing symptoms and emotional stress for patients and families.
Rectal cancer treatment is provided under the expert care of Dr. Rajesh Shinde, who focuses on modern, evidence-based treatment plans that aim not only to cure cancer but also to preserve normal bowel function and improve quality of life.
With the help of advanced technology, including robotic surgery for rectal cancer, personalized chemotherapy, radiation therapy, and comprehensive follow-up care, patients receive complete support from diagnosis to recovery.
Understanding Rectal Cancer
Rectal cancer starts when the cells lining the rectum begin to grow in an uncontrolled manner. These abnormal cells form a tumor which may grow locally or spread to nearby organs or distant parts of the body if not treated on time.
Most rectal cancers develop slowly and often begins as small growths called polyps. Over time, these polyps may turn cancerous. Regular screening can detect these changes early, making treatment easier and more successful.
Stages of Rectal Cancer
Stage 0: Cancer is only in the inner lining of the rectum and has not spread deeper.
Stage 1: Cancer has grown into the rectal wall but has not spread to lymph nodes.
Stage 2: Cancer has grown through the rectal wall but has not spread to lymph nodes.
Stage 3: Cancer has spread to nearby lymph nodes and surrounding tissues.
Stage 4: Cancer has spread to distant organs such as the liver or lungs.
Causes and Risk Factors of Rectal Cancer
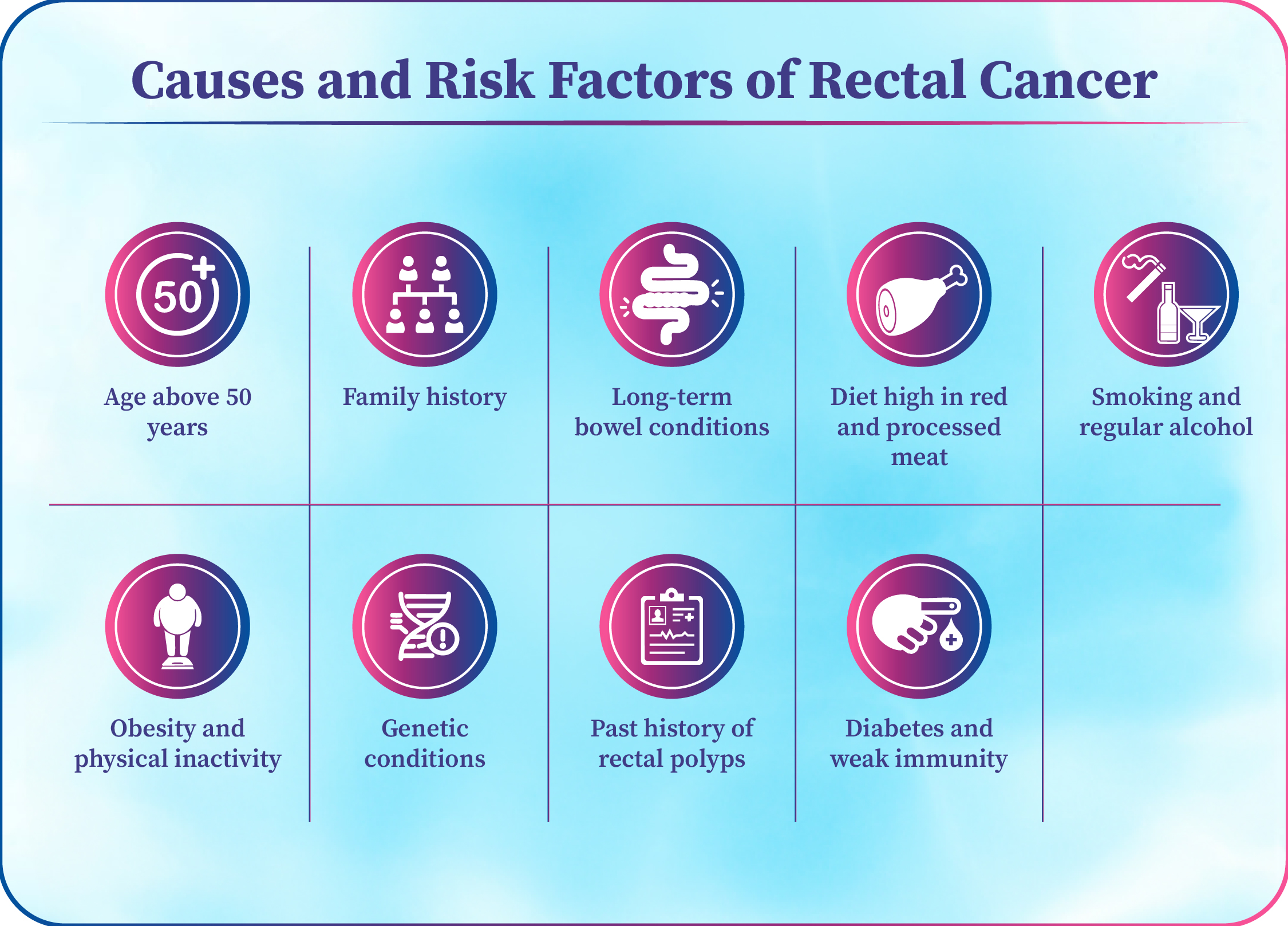
The exact cause of rectal cancer is not always known, but certain factors increase the risk.
Age above 50 years is a common risk factor for rectal cancer.
Family history of rectal or colorectal cancer raises the chances of developing the disease.
Long-term bowel conditions like ulcerative colitis and Crohn’s disease increase rectal cancer risk.
Diet high in red and processed meat and low in fiber is linked to rectal cancer.
Smoking and regular alcohol use are important lifestyle risk factors.
Obesity and physical inactivity increase the risk of rectal cancer.
Genetic conditions like FAP and Lynch syndrome raise rectal cancer risk at a younger age.
Past history of colon or rectal polyps increases future risk.
Diabetes and weak immunity may also increase rectal cancer risk.
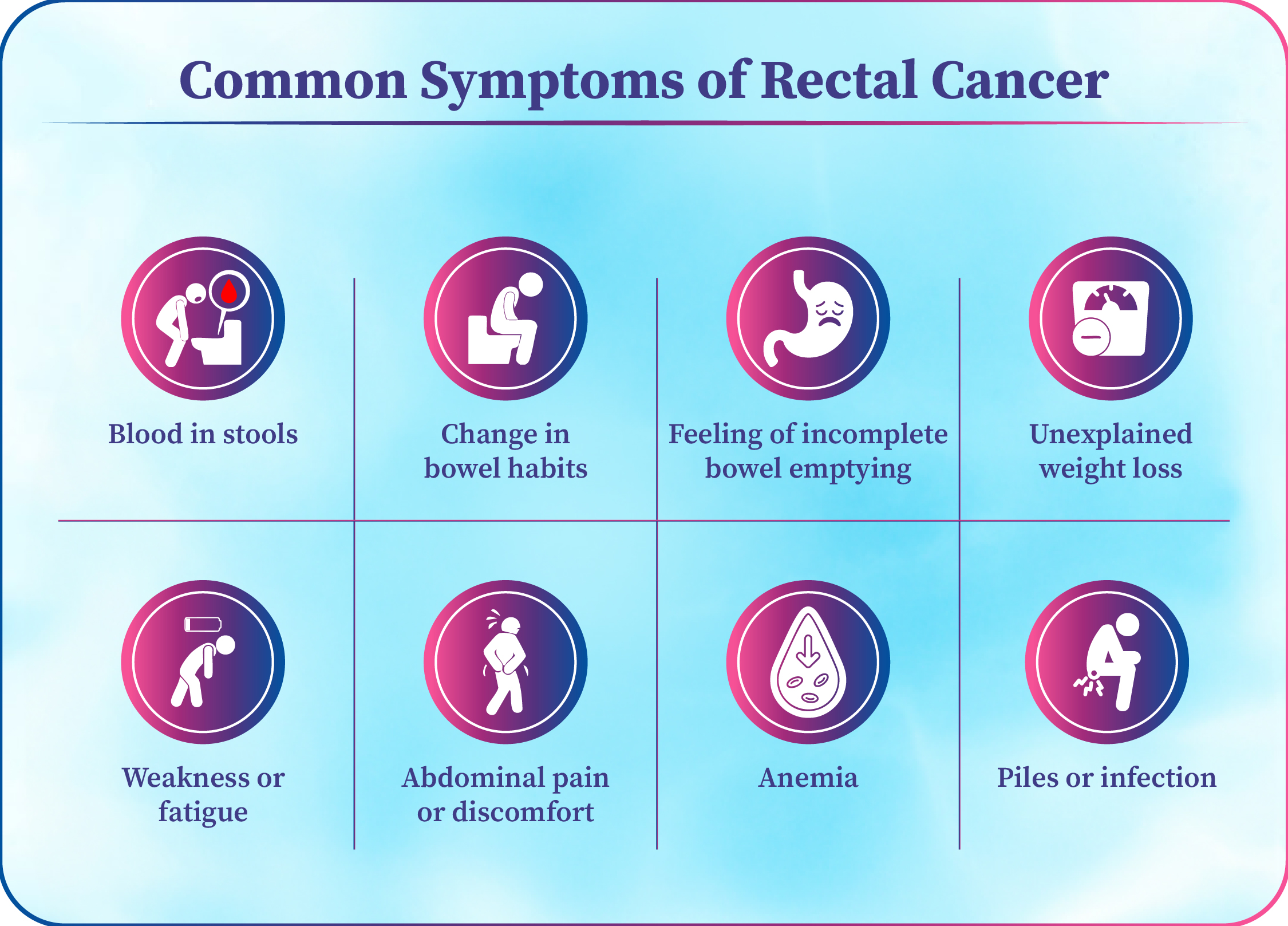
Common Symptoms of Rectal Cancer
Blood in stools
Change in bowel habits such as constipation or diarrhea
Feeling of incomplete bowel emptying
Unexplained weight loss
Weakness or fatigue
Abdominal pain or discomfort
Anemia due to long-term blood loss
Symptoms may look like piles or infection and should not be ignored.
Diagnosis of Rectal Cancer
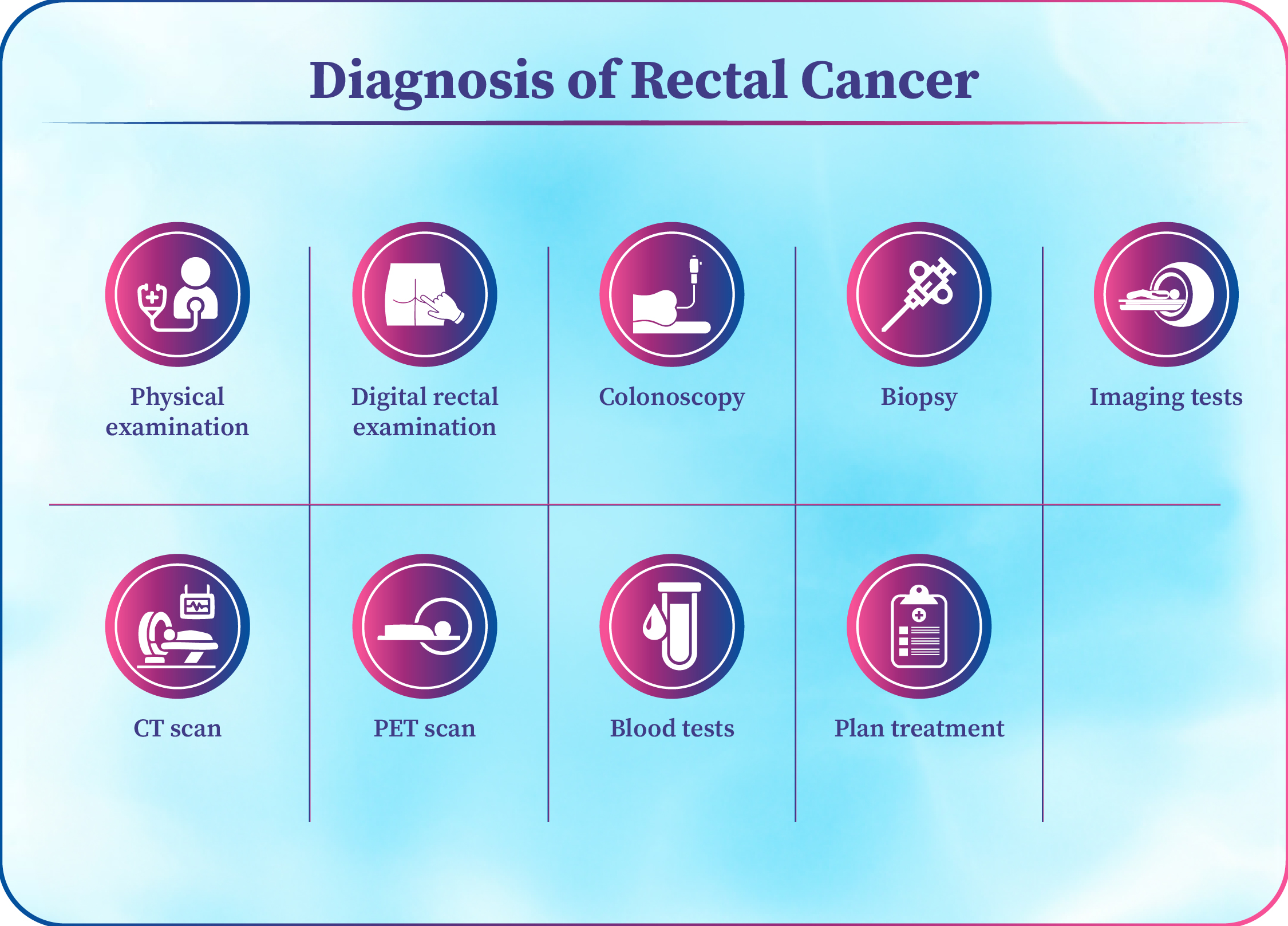
Diagnosis begins with a detailed medical history and physical examination.
Digital rectal examination may be done to feel for any abnormal growth.
Colonoscopy is the main test used to view the rectum and colon directly.
A biopsy is taken during colonoscopy to confirm the presence of cancer cells.
Imaging tests such as MRI of the pelvis help assess tumor size and spread.
CT scan of the chest and abdomen is done to check for spread to other organs.
PET scan may be advised in selected cases for further evaluation.
Blood tests, including tumor markers, help support diagnosis and monitoring.
These tests help determine the stage of rectal cancer and plan treatment.
Treatment Options for Rectal Cancer
Rectal cancer treatment is not the same for every patient. It depends on the stage of cancer, tumor location, overall health, and patient preferences. Treatment usually involves a combination of surgery, chemotherapy, and radiation therapy.
The main aim is to remove the tumor completely while preserving normal bowel and bladder function whenever possible.
Surgery for Rectal Cancer:
Surgery is the primary treatment for most rectal cancers. The goal is to remove the tumor along with nearby lymph nodes to prevent recurrence.In earlier times, surgery often resulted in permanent colostomy bags. Today, with advanced surgical techniques, most patients can avoid this and maintain natural bowel movement.Dr. Rajesh Shinde specializes in modern rectal cancer surgeries that focus on precision and function preservation.
Robotic Surgery for Rectal Cancer:
Robotic surgery is one of the most advanced methods for treating rectal cancer. It uses robotic arms controlled by the surgeon through a console. This allows extremely precise movements in the narrow pelvic area where the rectum is located.Robotic surgery for rectal cancer offers several benefits. It provides better visibility of the tumor and surrounding nerves, helps in more accurate tumor removal, reduces blood loss, causes less pain, and shortens hospital stay. Patients also recover faster and return to daily activities sooner.Robotic surgery is especially useful for low rectal tumors where preserving the anal muscles is important. This helps maintain normal bowel control and avoids permanent stomas whenever possible. Robotic rectal cancer surgery is performed by Dr. Rajesh Shinde using internationally accepted surgical protocols.
Chemotherapy for Rectal Cancer
Chemotherapy uses special medicines to kill cancer cells or stop their growth. It may be given before surgery to shrink the tumor or after surgery to destroy any remaining cancer cells.Some patients receive chemotherapy along with radiation therapy, called chemo radiation. This combination improves treatment success in many cases.The type and duration of chemotherapy depend on cancer stage and patient tolerance. Side effects are managed carefully with supportive care.
Radiation Therapy for Rectal Cancer
Radiation therapy uses high-energy rays to target cancer cells in the rectum. It is often used before surgery to reduce tumor size or after surgery to prevent recurrence.Modern radiation techniques are precise and minimize damage to nearby organs like the bladder and small intestine.
Personalized Treatment Planning
Rectal cancer treatment works best when it is planned by a multidisciplinary team. This includes surgical oncologists, medical oncologists, radiation specialists, radiologists, and nutrition experts.Dr. Rajesh Shindebelieves that every patient deserves a customized plan based on scientific evidence and individual needs
Life After Rectal Cancer Treatment
Recovery continues even after surgery or chemotherapy is completed.
Regular follow-up visits are needed to detect recurrence early.
Bowel habits may change and need long-term management.
Proper nutrition helps improve strength and healing.
Emotional and mental health support is important for recovery.
With proper care, most rectal cancer survivors can live normal, healthy lives.
Why Choose Dr. Rajesh Shinde for Rectal Cancer Treatment?
Dr. Rajesh Shinde is known for his expertise in gastrointestinal cancers, particularly rectal and colorectal cancers. His approach combines medical excellence with compassionate care.Patients benefit from advanced technology like robotic surgery, evidence-based treatment protocols, and continuous support throughout the cancer journey.His focus is not only on survival but also on preserving dignity, function, and quality of life.
Rectal cancer is a life-changing diagnosis, but with early detection and expert treatment, it is highly manageable. Modern advancements like robotic surgery, combined with personalized care, have transformed outcomes for patients.
Under the care of Dr. Rajesh Shinde, patients receive advanced rectal cancer treatment that focuses on cure, comfort, and long-term well-being. From diagnosis to recovery, every step is guided with expertise, transparency, and compassion.
If you or your loved one is facing rectal cancer, seeking timely care can make all the difference. With the right doctor, technology, and support, a healthy future is possible.
Faq's